Understanding US Healthcare Affordability: What Millions of Eligibility Checks Reveal About Patient Cost Exposure
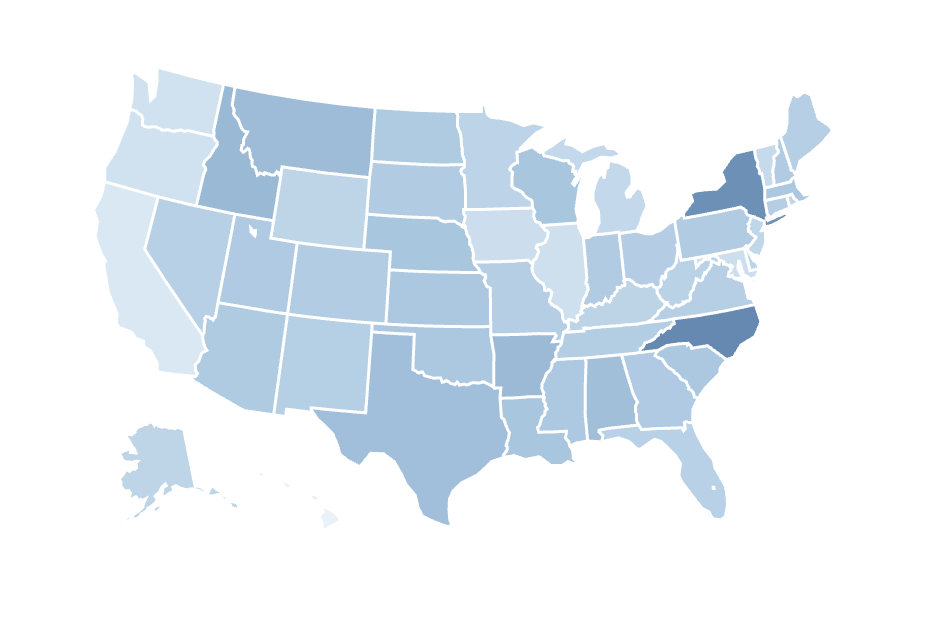
For this piece, we’ve chosen to present the data on a state-by-state basis, showing the average across government and commercial plans within each state. This approach allows us to highlight national trends and patterns that we have observed.
Read article



.png)







.png)